6. Stress Management & Inflammation

Chronic Inflammation and Neuroprogression in the Pathophysiology in Major Depression (Gollo Bertollo, et al, 2026) Given the inflammatory basis of MDD, treatment should extend beyond traditional monoaminergic therapies. Emerging approaches, including ketamine and monoclonal antibodies targeting inflammatory pathways, show promise.
Inflammation, stress and depression: An exploration of ketamine’s therapeutic profile (Johnston, et al, 2026)
Chronic stress, depression and inflammation have been consistently linked.
Stress-induced inflammatory states can contribute to treatment resistance.
Ketamine could be uniquely placed to target inflammation.
Ketamine’s effects can be mediated through the HPA axis or kynurenine pathway.
Anti-inflammatory antidepressant therapies could improve treatment resistance.
This study found that in cases of PTSD, while clients make psychological improvements, underlying inflammation may remain. If left untreated, psychological symptoms could be expected to return.
Peripheral inflammation over the course of a cognitive behavioral intervention in PTSD (2023)
PTSD symptoms decrease significantly in the course of cognitive behavioral therapy (CBT).
Inflammation (CRP) do not change significantly during CBT in PTSD patients.
This review of 23 studies found in cases of depression, there is a signal suggesting cognitive behavioral therapy affects certain biomarkers of stress.
Cognitive behaviour therapy and inflammation: A systematic review
of its relationship and the potential implications for the treatment of
depression (Lopresti, 2017).
A total of 23 studies investigating the anti-inflammatory effects of cognitive behaviour therapy were identified.
In 14 of these studies, at least one reduction in an inflammatory marker was reported, increases were identified in three studies and no change was found in six studies. Three studies examined the relationship between change in inflammation
and change in depressive symptoms following cognitive behaviour therapy. In two of these studies, change in depressive symptoms was associated with a change in at least one inflammatory marker. Finally, three studies examined the influence of pre-treatment inflammation on treatment outcome from cognitive behaviour therapy, and all indicated a poorer treatment response in people with higher premorbid inflammation.
When CBT isn't having the predicted effect, this may be an indication for pre-existing inflammation. This would be an indication for referral to a ketamine specialist for possible assessment for ketamine therapy.
At this point we continue learning and practicing cognitive behavioral mind body practice and monitor mood assessment scores. A medical provider may ask for labs for markers of inflammation in your system. How are you feeling in your body? What risk factors in your daily life increase the likelihood of underlying inflammatory responses, such as cortisol levels?

Cognitive-Behavioral Treatments for Anxiety and Stress-Related Disorders (Curtiss, et al, 2021) "Cognitive-behavioral therapy (CBT) is a first-line, empirically supported intervention for anxiety disorders. CBT refers to a family of techniques that are designed to target maladaptive thoughts and behaviors that maintain anxiety over time."
Body Scan Meditation for Stress
Body scan meditation helps you become more aware of stress and tension in your body.You can practice body scan meditation by lying down and focusing on each part of your body. Practicing body scan meditation regularly can reduce stress and improve your health.
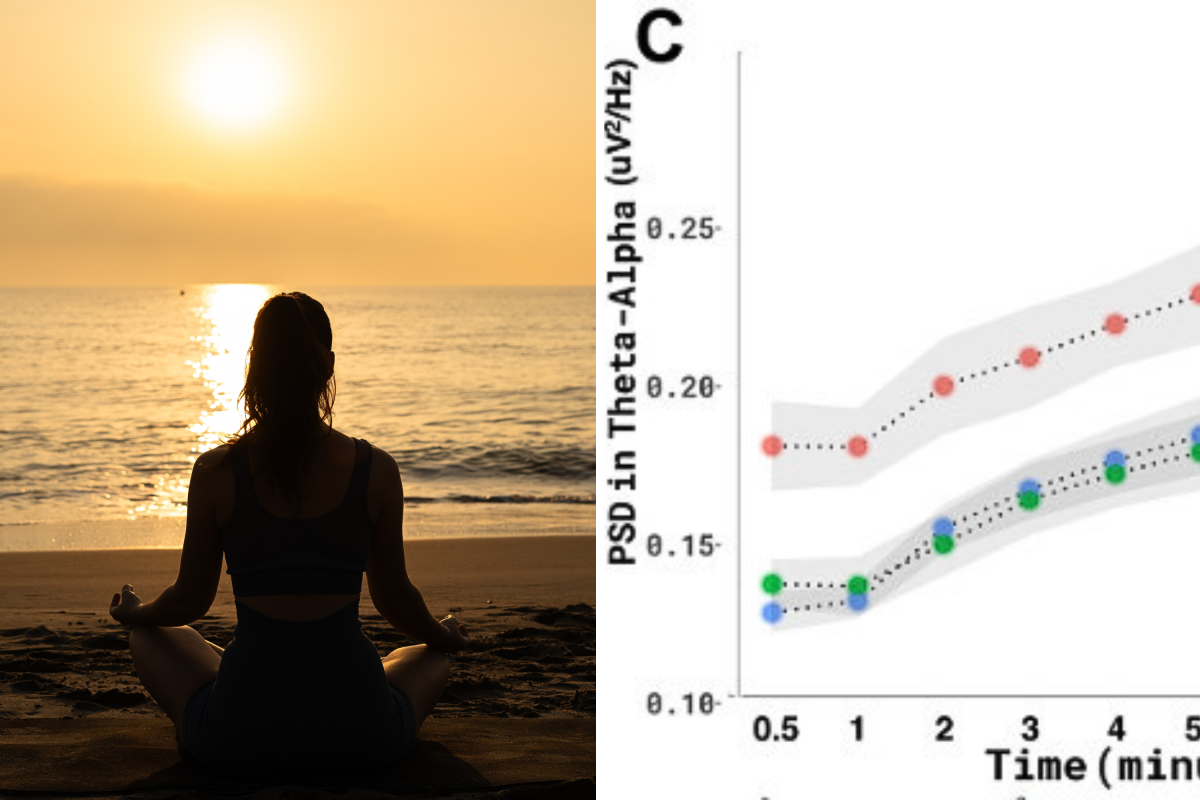
a new study, has proven that meditation can change the brain in just two–three minutes —and that even complete beginners can feel a brainwave shift after this interval.
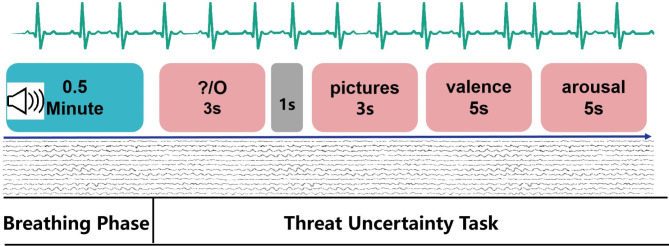
The effect of slow breathing in regulating anxiety (2025) "The results of showed that: Slow breathing effectively reduced anxiety, the valence and arousal are lower under the slow breathing..."
2026: "Our study suggests that the brain's response to meditation can be rapid and varies with practitioners’ experience, potentially influencing cognitive and emotional processing in significant ways."

(2026):"psilocybin has achieved 60-80% long-term remission of cancer-related depression and anxiety and peri-palliative ketamine studies demonstrate rapid but short-lived symptom control. In preclinical models these agents appear to normalize hypothalamic-pituitary-adrenal (HPA) axis function while upregulating neurotrophic factors, mechanisms which putatively promote stress reductions and resilience."


Ketamine as a potential cognitive enhancer in neurological disorders: evidence from preclinical and clinical studies (Rojas, et al, 2026)

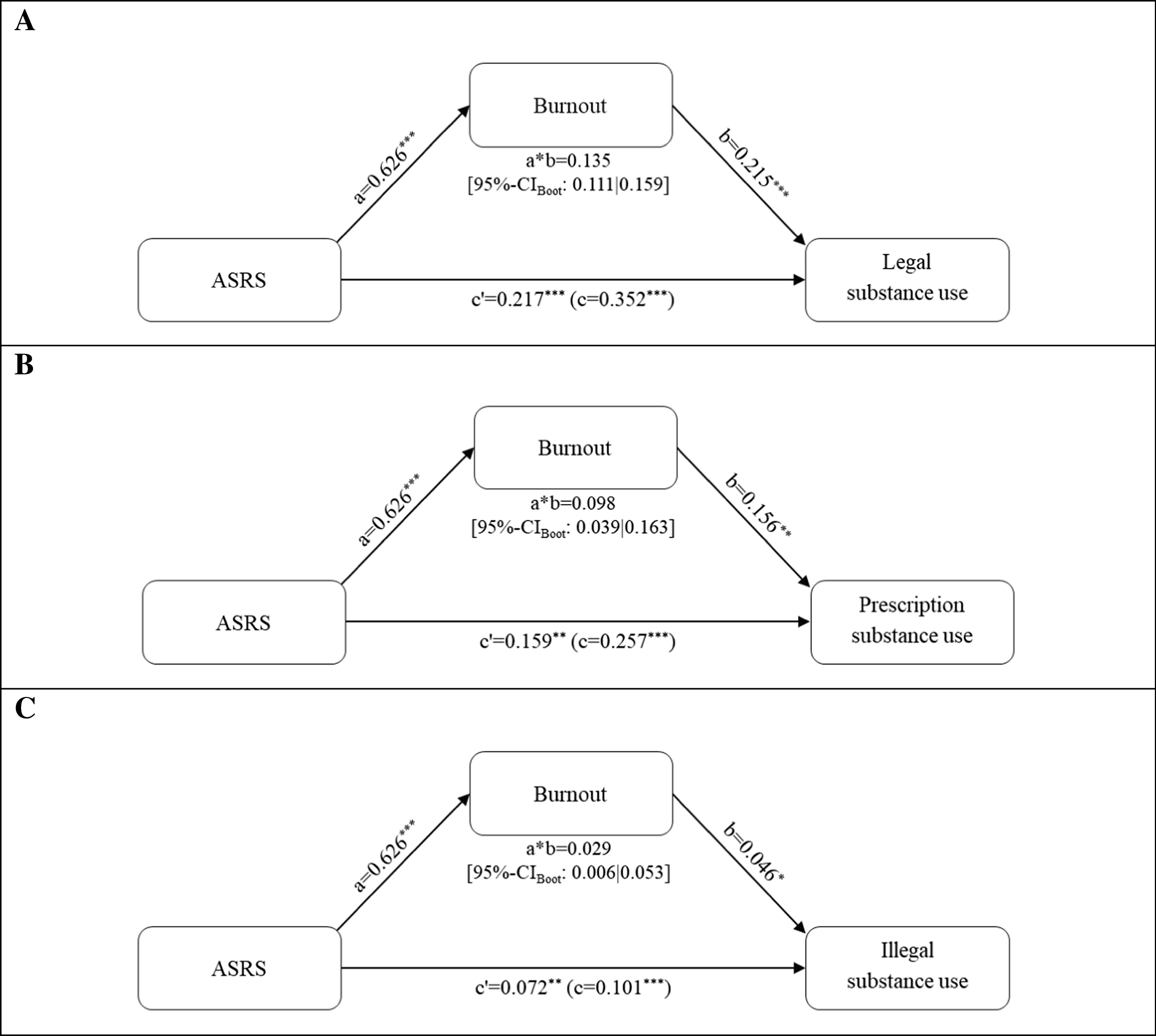
Under pressure: burnout as a pathway linking attention-deficit/hyperactivity disorder symptoms to substance-based cognitive enhancement use (2026) From a stress and health perspective, these findings are consistent with the view that burnout may function as a stress-related mechanism linking ADHD symptomatology to maladaptive coping behaviours in the workplace. This interpretation highlights the potential value of early identification and support for employees experiencing ADHD-related difficulties, in order to mitigate stress exposure and reduce reliance on potentially health-risky substance-based coping strategies
(2026):"The study reveals that under normal conditions, stress signals actually help us stay flexible and make good decisions. However, alcohol “cuts the wire” to this system, trapping the brain in rigid, habitual behaviors and explaining why stress is such a universal trigger for addiction and relapse."
NEUROPLASTICITY AND EMOTIONAL INTELLIGENCE: A PATHWAY TO COGNITIVE RESILIENCE (2026) “Findings demonstrate cultivating emotional intelligence through mindfulness, cognitive behavioral techniques, and social-emotional learning promotes beneficial neuroplastic changes enhancing cognitive resilience.” #mentalhealth #ketamine #psychedelics https://www.researchgate.net/publication/4


"people who are emotionally dysregulated experience high levels of stress and anxiety that can lead to poor physical and mental health. Some of the conditions associated with emotional dysregulation include being more sedentary, being overweight, and having high blood pressure and other stress-related problems."


Review

Review

Review

Review - DO an ABC exercise when you working on a trigger
The 90 Seconds of feeling triggered
"When you get the feeling that you are not safe, how does it feel inside of your body? ... sidestep your emotional reactivity when you feel triggered, so you can ground yourself in the present moment."
Treating job-related stress with psychedelic group therapy: a case series on group ketamine-assisted psychotherapy for healthcare workers and first responders (2025) KAP in group settings may offer a rapid reduction in depression, anxiety, and trauma-related symptoms. Adverse events were rare. This psychedelically oriented treatment model may represent a viable intervention for epidemic job-related stress in the healthcare workplace and larger controlled studies are warranted.

Chronic Pain and Major Depression: Shared Psychological and Neurobiological Mechanism (Lee, et al, 2026) Depression and chronic pain frequently co-occur, amplifying disease burden and complicating treatment. Shared mechanisms span immune, neurotransmitter, and neuroplastic domains. Neuroinflammation, characterized by elevated cytokines such as IL-6 (interleukin-6) and TNF-α (tumor necrosis factor-alpha), drives both mood dysregulation and nociplastic pain through microglial activation and central sensitization. Dysregulation of glutamate and gamma-aminobutyric acid (GABA) signaling contributes to excitatory-inhibitory imbalance, while altered BDNF (brain-derived neurotrophic factor) expression links neuroplasticity with pain amplification. Substance P and monoamine disturbances further integrate affective and somatic symptoms. Neuroimaging reveals overlapping dysfunction in prefrontal, cingulate, and limbic networks, providing a unifying framework for pain-emotion interactions. Psychological and social factors, including maladaptive cognitions, emotion regulation deficits, and reduced social support, exacerbate this bidirectional relationship. Clinically, tricyclic antidepressants and SNRIs (serotonin-norepinephrine reuptake inhibitors) demonstrate superior analgesic efficacy compared with SSRIs, particularly in neuropathic pain, fibromyalgia, and irritable bowel syndrome. Novel agents such as ketamine and esketamine show rapid antidepressant and potential analgesic effects. Neuromodulation strategies (rTMS (repetitive transcranial magnetic stimulation), tDCS (transcranial direct current stimulation)) and psychological interventions (CBT (cognitive behavioral therapy), mindfulness, ACT (acceptance and commitment therapy)) further enhance outcomes. Together, these findings support a precision medicine approach that integrates biological, psychological, and social determinants. Targeting convergent mechanisms may reduce symptom burden, improve treatment responsiveness, and ultimately enhance quality of life in patients with comorbid depression and chronic pain.

New Antidepressant Development in the Treatment of Depression (Spiti, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/420365 "A breakthrough came with N-methyl-D-aspartate (NMDA) receptor antagonists such as ketamine and esketamine, which achieved fast-acting effects and shifted the focus to glutamatergic modulation. Other developments in this area include modulators such as partial agonists, positive allosteric modulators (PAMs), and negative allosteric modulators (NAMs). In addition, gamma-aminobutyric acid (GABA) modulation has gained attention, with neurosteroids such as zurolone (approved for postpartum depression [PPD]) representing a new therapeutic approach. Other new strategies target the opioid system, particularly kappa-opioid receptor (KOR) antagonism, whose role in the treatment of anhedonia and depression is being investigated. Psychedelics, including psilocybin, have come back into focus as potential treatments due to their ability to elicit rapid and sustained antidepressant effects via agonism of the serotonin 2A receptor (5-HT2A)"

Try an ABC exercise









