Ketamine Research & Selected Bibliography
Ketamine Research
We're moving some things around to better serve our clinical and non-clinical members. Here are some selected studies to get started.
Become a Member


Jun 19, 2024Psychedelic Cognitive Behavioral Therapy (On Ketamine, Context and Competencies in "Assisted-Psychotherapy")
Jun 19, 2024
An evolving overview of cognitive behavioral therapy in modern psychedelic-assisted psychotherapy and ketamine psychedelic therapy See Preliminary Lit Review for more sources and summariesRead More →

Jun 8, 2024
A total of 251 patients were randomized (median age, 51 [IQR, 34-69] years; 111 women [44.9%] and 140 men [55.1%] among the 247 with data available) and were included in the intention-to-treat population. The mean pain score change was −3.7 (95% CI, −4.2 to −3.2) in the ketamine group compared with −3.8 (95% CI, −4.2 to −3.4) in the morphine group. The difference in mean pain score change was 0.1 (95% CI, −0.7 to 0.9) points. There were no clinically meaningful differences for vital signs between the 2 groups. The intravenous morphine group had 19 of 113 (16.8% [95% CI, 10.4%-25.0%]) adverse effects reported (most commonly nausea [12 of 113 (10.6%)]) compared with 49 of 120 (40.8% [95% CI, 32.0%-49.6%]) in the ketamine group (most commonly emergence phenomenon [24 of 120 (20.0%)]). No adverse events required intervention.
Conclusions and Relevance In the KETAMORPH study of patients with out-of-hospital traumatic pain, the use of intravenous ketamine compared with morphine showed noninferiority for pain reduction. In the ongoing opioid crisis, ketamine administered alone is an alternative to opioids in adults with out-of-hospital traumatic pain.Read More →
Jun 8, 2024
The MUSIK trial found that music significantly decreased ketamine-induced systolic BP changes. Music may thus represent a feasible, benign, nonpharmacological approach to improving the hemodynamic response of subanesthetic ketamine infusions for TRD. Secondary trial outcomes will be published elsewhere.
Beyond psychiatric contexts, the stimulatory hemodynamic effects of ketamine have received extensive study, both as desirable (eg, in surgical contexts) and as potentially harmful (eg, in procedural sedation),5 but never in relation to music, to our knowledge. The magnitude of the hemodynamic effects observed in this study suggests that ketamine research should consider potential influences of contextual factors, including auditory stimuli. Ketamine’s unique psychoactive effects may amplify the effects of music and other environmental influences, as has been long observed in the anesthesiology literature.6
Although the MUSIK trial administered 181 ketamine infusions, its modest sample size is a limitation. Further investigation is needed in larger samples and additional clinical contexts.Read More →
Jun 1, 2024
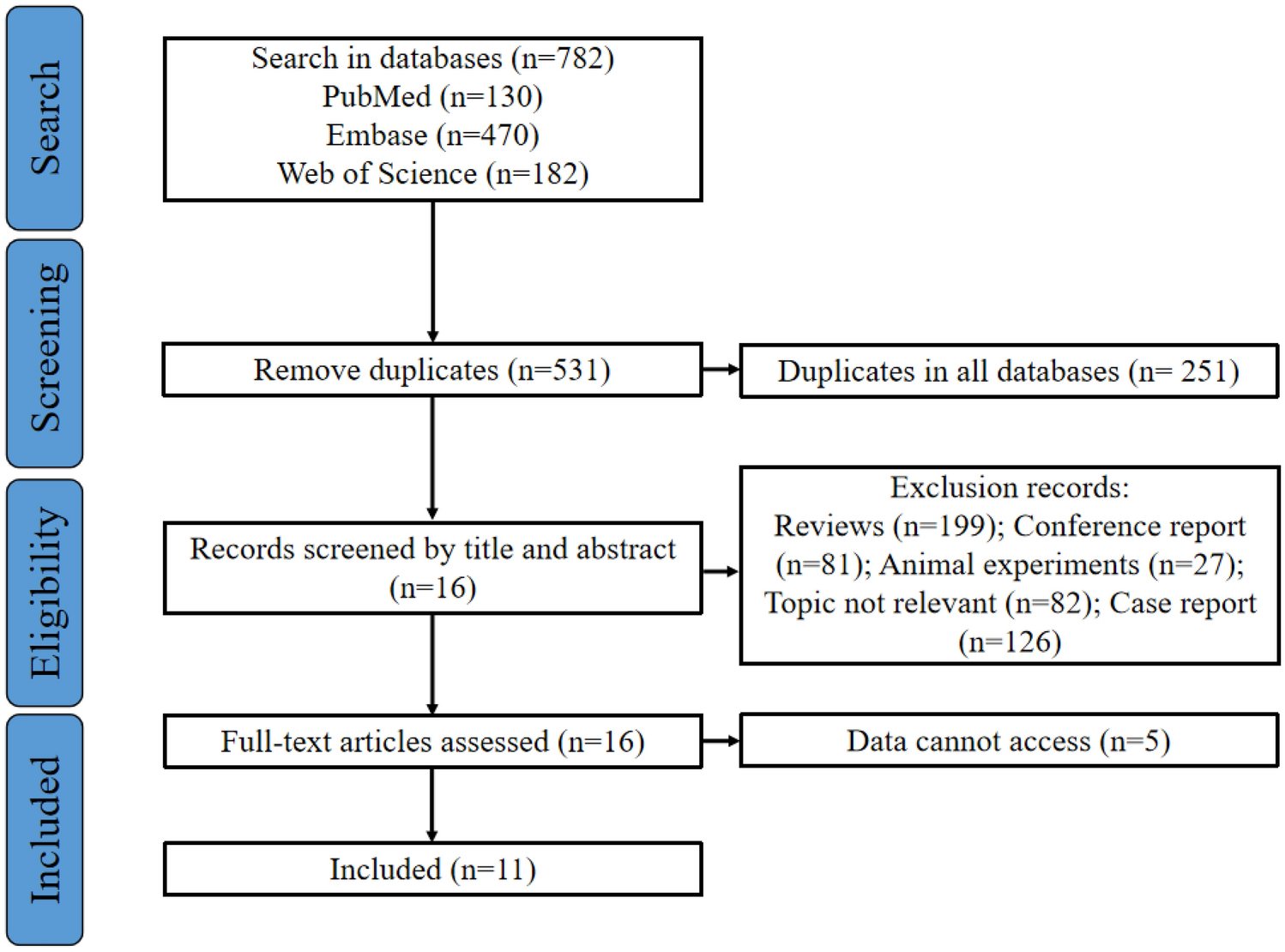
Out of 782 studies retrieved from electronic databases, 11 met the inclusion criteria. Among them, 10 studies were retrospective, and 1 study was prospective. Patient data for inclusion were sourced from the case registries of the researchers' respective hospitals. Across all included studies, the administration of ketamine significantly reduced the duration of status epilepticus and demonstrated higher safety compared to patients not receiving ketamine treatment for super-refractory status epilepticus. Additionally, early administration of ketamine correlated with improved treatment outcomes. The risk of bias across all studies was deemed low.Read More →

May 30, 2024
Researchers write “A sample of 11,441 patients was analyzed, At-home, telehealth-supported ketamine administration was largely safe, well-tolerated, and associated with improvement in patients with depression. Strategies for combining psychedelic-oriented therapies with rigorous telehealth models, as explored here, may uniquely address barriers to mental health treatment.” Read More →
May 13, 2024 Can Ketamine-Induced Near-Death Experiences Expedite Healing? (Sienknecht, 2020)

The potential for ketamine to replicate NDE’s has been supported by research. A recent study published in Science Direct, looking at over 15,000 self-reports, found that the use of ketamine, over all other psychedelic compounds, most frequently led users to have NDE’s (followed by salvia in second and peyote in third). “After assessing the semantic similarity between 15,000 reports linked to the use of 165 psychoactive substances and 625 NDE narratives, we determined that the N-methyl-D-aspartate (NMDA) receptor antagonist ketamine consistently resulted in reports most similar to those associated with NDE’s.” The authors go on to suggest that “ketamine could be used as a safe and reversible experimental model for NDE phenomenology”1 Read More →
Within 1 h of ketamine dosing, patients reported reduced depression and anxiety ratings, which persisted for up to 7 days. A dose–response profile for ketamine was noted for dissociative side effects, adverse events and changes in blood pressure; however, changes in mood ratings were broadly similar for both ketamine doses. Overall, 14/25 patients (56%) were responders (⩾50% reduction at 24 h compared with baseline) for either ketamine dose for the Hospital Anxiety and Depression Scale (HADS), and 18/25 (72%) were responders for the HADS-anxiety scale. After fentanyl, only 1/25 (HADS-depression) and 3/25 (HADS-anxiety) were responders. Ketamine was generally safe and well tolerated in this population.
Conclusions:
Our findings add to the literature confirming ketamine’s activity against depressive and anxiety symptoms in patients with TRD.Read More →
This scoping review describes the existing literature on the joint use of music and ketamine-or esketamine (the S(+) enantiomer of ketamine)-in humans. The review considers that extant studies have explored the intersection of ketamine/esketamine and music in healthy volunteers and in patients of various age groups, at different dosages, through different treatment processes, and have varied the sequence of playing music relative to ketamine/esketamine administration.Read More →
May 2, 2024Cognitive behavioral therapy in psychedelic-assisted psychotherapy (an ongoing review, part 1)
May 2, 2024
An evolving overview of cognitive behavioral therapy in psychedelic-assisted psychotherapy and ketamine psychedelic therapy.Read More →
Apr 20, 2024
Esketamine and psilocybin NNT (number to treat) suggests safety and efficacy for depressionRead More →
KETAMINE THERAPY RESEARCH & SELECTED BIBLIOGRAPHY:
Over 60 years of research exists on racemic ketamine, a generic medicine that was FDA approved in humans and animals safe up to very high doses in humans and animals in medical emergencies, surgery as an anesthetic, and at sub-anesthetic doses, is a psychedelic medicine that has been studied in mental health and pain disorders. It has been prescribed at various doses for various use-cases by providers around the world for decades.
Ketamine in neuropsychiatric disorders: an update (Johnston, et al, 2023)
Subtypes of the psychedelic experience have reproducible and predictable effects on depression and anxiety symptoms (Nikolaidis, et al, 2023)
A transdiagnostic systematic review and meta-analysis of ketamine’s anxiolytic effects (Hartland, et al, 2023)
Classical and non-classical psychedelic drugs induce common network changes in human cortex (Dal, et al, 2023)
Ketamine for the treatment of major depression: a systematic review and meta-analysis (Nikolin, et al, 2023)
Maintenance ketamine treatment for depression: a systematic review of efficacy, safety, and tolerability (Apeldoorn, et al, 2022)
Depression and antidepressant effects of ketamine and its metabolites: The pivotal role of gut microbiota (Hua, 2022)
Ketamine and its metabolites: Potential as novel treatments for depression (Zhang, 2022)
The effect of IV ketamine in patients with major depressive disorder and elevated features of borderline personality disorder (Chen, et al, 2022)
Gender differences in the antianhedonic effects of repeated ketamine infusions in patients with depression (Zheng, 2022)
An Expert-Informed Introduction to the Elements of Psychedelic-Assisted Therapy (Brainfutures, 2022)
Ketamine may exert rapid antidepressant effects through modulation of neuroplasticity, autophagy, and ferroptosis in the habenular nucleus (Zhang, et al, 2022)
Evaluation of Early Ketamine Effects on Belief-Updating Biases in Patients With Treatment-Resistant Depression (Bottemann, et al, 2022)
Safety, effectiveness and tolerability of sublingual ketamine in depression and anxiety: A retrospective study of off-label, at-home use (Hassan, et al, 2022)
Real-world depression, anxiety and safety outcomes of intramuscular ketamine treatment: a retrospective descriptive cohort study (Ahuja, et al, 2022)
Towards an understanding of psychedelic-induced neuroplasticity (Calder & Hasler, 2022)
Neurobiological, behavioral, and cognitive effects of ketamine in adolescents: A review of human and pre-clinical research (Acevedo, et al, 2022)
Ketamine for suicidality: An umbrella review (Shamabadhi, et al, 2022)
Ketamine induces rapid antidepressant effects via the autophagy-NLRP3 inflammasome pathway (Lyu, et al, 2022)
Active mechanisms of ketamine-assisted psychotherapy: A systematic review (Joneborg, 2022)
Psychedelic integration: An analysis of the concept and its practice (Bathje, et al, 2022)
Comparison of psychedelic and near-death or other non-ordinary experiences in changing attitudes about death and dying (Sweeney, et al, 2022)
Magnetoencephalography biomarkers of suicide attempt history and antidepressant response to ketamine in treatment-resistant major depression (Gilbert, 2022)
Ketamine Augmented Psychotherapy (KAP) in mood disorder: User guide (Bottemanne et al, 2022)
Low addiction risk with medical use of ketamine: Animal study (2022)
A short burst of reward curbs the addictiveness of ketamine (2022)
The abuse liability of ketamine: A scoping review of preclinical and clinical studies (Le, et al, 2022)
Ketamine Assisted Psychotherapy: A Systematic Narrative Review of the Literature (Drozdz et al, 2022)
Ketamine for Bipolar Depression: Biochemical, Psychotherapeutic, and Psychedelic Approaches (Bennett et al, 2022)
Psychedelic assisted therapy for major depressive disorder: Recent work and clinical directions (McCartney, et al, 2022)
Sustained effects of single doses of classical psychedelics in humans (2022)
A Systematic Review of Neurocognitive Effects of Subanesthetic Doses of Intravenous Ketamine in Major Depressive Disorder, Post-Traumatic Stress Disorder, and Healthy Population (Shiroma, et al 2022)
Ethnoracial Inclusion in Clinical Trials of Ketamine in the Treatment of Mental Health Disorders (Michaels, et al, 2022)
A case series of group-based ketamine-assisted psychotherapy for patients in residential treatment for eating disorders with comorbid depression and anxiety disorders (Robison & LaFrance, 2022)
Real-world effectiveness of ketamine in treatment-resistant depression: A systematic review & meta-analysis (Alnefeesi, et al, 2022)
Psychedelics, Mystical Experience, and Therapeutic Efficacy: A Systematic Review (2022)
Buddhist-like opposite diminishing and non-judging during ketamine infusion are associated with antidepressant response: an open-label personalized-dosing study (Stocker et al, 2022)
Psychedelics and Psychotherapy: Cognitive-Behavioral Approaches as Default (2022)
Toward Synergies of Ketamine and Psychotherapy (2022)
Long-term safety of ketamine and esketamine in treatment of depression (2022)
Oral ketamine reduces the experience of stress in people with chronic suicidality (2022)
Brain Changes Associated With Long-Term Ketamine Abuse, A Systematic Review (Strous, et al 2022)
A retrospective analysis of ketamine intravenous therapy for depression in real-world care settings (2022)
Adjunctive Ketamine With Relapse Prevention-Based Psychological Therapy in the Treatment of Alcohol Use Disorder (Grabski, et al, 2022)
Mechanisms of ketamine and its metabolites as antidepressants (Hess,et al, 2022)
Ketamine for the treatment of mental health and substance use disorders: comprehensive systematic review (Walsh, et al, 2022)
Gut microbiota is involved in the antidepressant-like effect of (S)-norketamine in an inflammation model of depression (Wang, et al, 2021)
Low dose oral ketamine treatment in chronic suicidality: An open-label pilot study (Can, et al, 2021)
Ketamine Treatment for Depression in Patients With a History of Psychosis or Current Psychotic Symptoms: A Systematic Review (Veraart, et al, 2021)
The effectiveness, safety and tolerability of ketamine for depression in adolescents and older adults: A systematic review (Di Vincinzo, et al, 2021)
Six-week oral ketamine treatment for chronic suicidality is associated with increased grey matter volume (Gallay, 2021)
Ketamine-Assisted Psychotherapy for PTSD Related to Racial Discrimination (Halstead, et al, 2021)
Ketamine-assisted psychotherapy for trauma-exposed patients in an outpatient setting: A clinical chart review study (Davis, et al, 2021)
Cognitive Behavioral Therapy to Sustain the Antidepressant Effects of Ketamine in Treatment-Resistant Depression: A Randomized Clinical Trial (Wilkinson et aL, 2021)
A Potential Case of Acute Ketamine Withdrawal: Clinical Implications for the Treatment of Refractory Depression (Roxas, et al 2021)
Neuroplasticity as a convergent mechanism of ketamine and classical psychedelics (2021)
Ancient Roots of Today's Emerging Renaissance in Psychedelic Medicine (2021)
Can Ketamine be taken orally? (2021)
Ketamine’s Role in Spirituality: How One Synthetic Drug Catalyzes a Natural Experience (Woods, 2021)
Ketamine specifically reduces cognitive symptoms in depressed patients: An investigation of associated neural activation patterns (Stippl et al, 2021)
Long-term safety and efficacy of sublingual ketamine troches/lozenges in chronic non-malignant pain management (Maudlin et al, 2021)
Predicting Reactions to Psychedelic Drugs: A Systematic Review of States and Traits Related to Acute Drug Effects (Adal, et al, 2021)
Same But Different: Antidepressant Mechanisms of Psilocybin and Ketamine (Gallenstein, 2021)
Intranasal Ketamine for Depression in Adults: A Systematic Review and Meta-Analysis of Randomized, Double-Blind, Placebo-Controlled Trials (An, et al, 2021)
Ketamine and Serotonergic Psychedelics: Common Mechanisms Underlying the Effects of Rapid-Acting Antidepressants (Kadriu, et al, 2021)
Pharmacokinetics of ketamine and its major metabolites norketamine, hydroxynorketamine, and dehydronorketamine: a model-based analysis (Kamp, et al, 2020)
Psychological flexibility mediates the relations between acute psychedelic effects and subjective decreases in depression and anxiety (Davis, et al, 2020)
Ketamine can be produced by Pochonia chlamydosporia: an old molecule and a new anthelmintic? (Ferreira et al, 2020)
GABA interneurons are the cellular trigger for ketamine's rapid antidepressant actions (Gerhard, et al, 2020)
Efficacy of single and repeated administration of ketamine in unipolar and bipolar depression: a meta-analysis of randomized clinical trials (Kryst et al, 2020)
An Update on the Efficacy and Tolerability of Oral Ketamine for Major Depression: A Systematic Review and Meta-Analysis (Nuñez et al, 2020)
Effects of Serial Ketamine Infusions on Corticolimbic Functional Connectivity in Major Depression (Vasavada, et al, 2020)
Oral Ketamine for Depression, 2: Practical Considerations (2019)
Efficacy of ketamine therapy in the treatment of depression (Mandal, et al, 2019)
Neurochemical models of near-death experiences: A large-scale study based on the semantic similarity of written reports (Martial, 2019)
The Efficacy of Ketamine in the Palliative Care Setting: A Comprehensive Review of the Literature (2019)
Oral Ketamine for Depression: A Systematic Review (Rosenblat et al, 2019)
Molecular and cellular mechanisms underlying the antidepressant effects of ketamine enantiomers and its metabolites (Yang, 2019)
The effects of ketamine on prefrontal glutamate neurotransmission in healthy and depressed subjects (Abdallah, et al, 2018)
Ketamine Assisted Psychotherapy (KAP): Patient Demographics, Clinical Data and Outcomes in Three Large Practices Administering Ketamine with Psychotherapy (Dore, et al, 2018)
Ketamine for Depression (Hyde, 2018)
Does oral administration of ketamine accelerate response to treatment in major depressive disorder? Results of a double-blind controlled trial (Arabzadeh 2018)
Impact of oral ketamine augmentation on hospital admissions in treatment-resistant depression and PTSD: a retrospective study (Hartberg, et al, 2018)
Psychedelics and reconsolidation of traumatic and appetitive maladaptive memories: focus on cannabinoids and ketamine (Fattore, et al, 2018)
Ketamine and Ketamine Metabolite Pharmacology: Insights into Therapeutic Mechanisms (Zanos, et al, 2018)
Side-effects associated with ketamine use in depression: a systematic review (Short et al, 2017)
Antidepressant drug action--From rapid changes on network function to network rewiring (2016)
Ketamine: 50 Years of Modulating the Mind (2016)
Ketamine safety and tolerability in clinical trials for treatment-resistant depression (Wan, et al, 2015)
A Rare Urachal Cyst in a Case of Ketamine-induced Cystitis Provides Mechanistic Insights (2015)
Ameliorating treatment-refractory depression with intranasal ketamine: potential NMDA receptor actions in the pain circuitry representing mental anguish (Opler, et al, 2015)
Ketamine Psychedelic Psychotherapy: Focus on its Pharmacology, Phenomenology, and Clinical Applications (Kolp 2014)
What is hydroxynorketamine and what can it bring to neurotherapeutics? (Singh,et al, 2014)
A randomized controlled trial of intranasal ketamine in major depressive disorder (Lapidus, 2014)
Ketamine: Use in Anesthesia (Marland, et al, 2013)
Ketamine Psychedelic Therapy (KPT): A Review of the Results of Ten Years of Research (Kolp 2011)
What did STAR*D teach us? Results from a large-scale, practical, clinical trial for patients with depression (Gaynes, et Al, 2009)
Development of a rational scale to assess the harm of drugs of potential misuse (Nutt & King, 2007)
Ketamine psychedelic therapy (KPT): a review of the results of ten years of research (Krupitsky 1997)
Ketamine and norketamine plasma concentrations after i.v., nasal and rectal administration in children (Malinovsky, et al, 1996)
Ketamine Psychotherapy: Results and Mechanisms (Krupitsky 1996)
Evaluation of ketamine HCl for anti-depressant activity (Sofia, 1975)
The Use of Ketamine in Psychiatry (Khorramzadeh, et al, 1973)
CLINICAL TRIAL OF KETAMINE (CI-581): A PRELIMINARY REPORT (Oduntan, et al,1970)
How Ketamine Drug Helps with Depression (2022)- "Most important for people to know… ketamine needs to be part of a more comprehensive treatment plan for depression.“Patients will call me up and say they don’t want any other medication or psychotherapy, they just want ketamine, and I have to explain to them that it is very unlikely that a single dose, or even several doses of ketamine alone, will cure their depression,” says Dr. Sanacora. Instead, he explains, “I tell them it may provide rapid benefits that can be sustained with comprehensive treatment plans that could include ongoing treatments with ketamine. Additionally, it appears to help facilitate the creation new neural pathways that can help them develop resiliency and protect against the return of the depression.”
This is why Dr. Sanacora believes that ketamine may be most effective when combined with cognitive behavioral therapy (CBT), a type of psychotherapy that helps patients learn more productive attitudes and behaviors. Ongoing research, including clinical trials, addressing this idea are currently underway at Yale."
See Also:Read More →
Jun 5, 2024
40 research articles were included for review: 26 studies on EBPI for PTSD, and 14 studies on PT. EBPI studied were CBT, EMDR, CPT and PE. Psychedelic compounds studied were psilocybin, ibogaine, LSD, MDMA and ketamine, for treatment of substance use disorders, anxiety relating to physical illness, depression, and PTSD. Core themes from patient experiences of EBPI: 1) patient burden in PTSD treatment; 2) readiness; 3) key mechanisms of change; 4) psychological safety and trust. Themes identified in the review of PT: 1) indirect trauma processing; 2) reorganisation of self-narratives via processes of relatedness and identification; 3) key treatment characteristics.
Conclusion: This study suggests overlap between patients' experience of EBPI and PT in terms of key mechanisms of change, the importance of psychological safety and readiness to engage in treatment. Trauma-informed care paradigms and practices may improve safety and acceptability of PT research.Read More →
Jun 2, 2024
The serotonin deficit hypothesis explanation for major depressive disorder (MDD) has persisted among clinicians and the general public alike despite insufficient supporting evidence. To combat rising mental health crises and eroding public trust in science and medicine, researchers and clinicians must be able to communicate to patients and the public an updated framework of MDD: one that is (1) accessible to a general audience, (2) accurately integrates current evidence about the efficacy of conventional serotonergic antidepressants with broader and deeper understandings of pathophysiology and treatment, and (3) capable of accommodating new evidence. In this article, we summarize a framework for the pathophysiology and treatment of MDD that is informed by clinical and preclinical research in psychiatry and neuroscience. First, we discuss how MDD can be understood as inflexibility in cognitive and emotional brain circuits that involves a persistent negativity bias. Second, we discuss how effective treatments for MDD enhance mechanisms of neuroplasticity-including via serotonergic interventions-to restore synaptic, network, and behavioral function in ways that facilitate adaptive cognitive and emotional processing. These treatments include typical monoaminergic antidepressants, novel antidepressants like ketamine and psychedelics, and psychotherapy and neuromodulation techniques. At the end of the article, we discuss this framework from the perspective of effective science communication and provide useful language and metaphors for researchers, clinicians, and other professionals discussing MDD with a general or patient audience.Read More →
Jun 2, 2024






