Cognitive Behavioral Mental Health & Psychedelics

Ketamine Psychedelic Preparation Guide (EN)
"Psychedelic" is a word coined in the middle of the 20th Century to describe the mind manifesting, soul-opening experiences elicited by chemical compounds including, but not limited to LSD, psilocybin, ketamine, esketamine, MDMA, DMT, cannabis, and mescaline. These experiences often result in great shifts in perspective, and are felt in ways people describe as mind, body, heart, and spirit.
Research suggests a cognitive behavioral, existential, mind-body approach offers a way to integrate and sustain these shifts to manage the inevitable stressors in your ongoing life, leaving room for wonder and meaning-making from the medicine experience, and the possibility of approaching obstacles differently and suffer less moving forward.



(2026): "Typical (or serotonergic) psychedelics (psilocybin, ayahuasca) and atypical (glutamatergic/NMDA) psychedelics (ketamine, esketamine). Both approaches, via a different entrance mechanism, have a fast (immediate) onset, combined with a long-lasting antidepressant action, which cannot be explained by long-term biological presence of the drug in the brain. The psychedelic drugs acutely initiate short-lasting CNS-induced side effects but also lead to activation of downstream cortical processes that underlie the 'lasting' antidepressant effects. In the present chapter, the clinical developments that have led to the marketing of psilocybin and esketamine for major depression disorders has been described. The emergence of fast onset antidepressants for major depression and treatment-resistant depression is a huge step forward in treating major psychiatric disorders."

(2026): "Ketamine, through blocking N-methyl-D-aspartate (NMDA) receptors, has established a new paradigm for rapid-acting antidepressant intervention..." Our review highlights the specific biological changes that drive these effects. Beyond monoamine regulation, key factors include modulation of glutamate and GABA signals, which contribute to the restoration of synaptic plasticity in damaged brain circuits. "

(2026):"findings indicate that cognitive-behavioral strategies have been incorporated into psychedelic-assisted interventions in diverse ways, across different phases of treatment and with distinct therapeutic purposes."
Ketamine combined with psychotherapy for treatment-resistant depression: Real-world outcomes and the role of subjective experience (Cohen, et al, 2026)

(2026):"Affective disorders such as depression, anxiety disorders and suicidality are major contributors to global psychiatry. The "chemical imbalance" theory has been traditionally used; however recent research suggests that neurotransmitter dysfunction may represent an important early contributor within a broader, bidirectional cascade of cellular changes. Stress responses and neural circuits are disrupted by dysregulation of the serotonergic, noradrenergic, dopaminergic, GABAergic, and glutamatergic systems, which leads to oxidative stress, excitotoxicity, neuroinflammation, and decreased trophic support. Reduced brain-derived neurotrophic factor (BDNF) signaling, dendritic retraction, synapse loss, and apoptotic susceptibility are the common pathways that result in both amygdala hyperactivity and structural atrophy in the hippocampus and prefrontal cortex. Rumination, fear, anhedonia, cognitive impairment, and suicidal ideation are clinical manifestations of the ensuing circuit failure. This study proposes a unified model of pathogenesis in which increasing cellular damage is driven by neurotransmitter dysregulation, integrating evidence from both the neurochemical and cellular domains. Reassessing the delayed but plasticity-enhancing benefits of SSRIs and SNRIs, the quick synaptic repair brought about by NMDA antagonists like ketamine, and the potential of new drugs that target oxidative stress, inflammation, and glutamate receptor subtypes are some of the therapeutic implications. Lastly, it is highlighted that developing biomarkers for oxidative damage and neuroinflammation is an essential next step in the development of precision psychiatry. This paradigm aims to shift the emphasis from regulating neurotransmitters to promoting cellular resilience and rebuilding brain circuits in order to re-imagine the future of treatment for depression, anxiety, and suicidality."

Mystical Experience Induced by Esketamine Treatment: A Real-World Observational Study (Mallevays, et al., 2026) https://pubmed.ncbi.nlm.nih.gov/41959772/ “These findings add to the growing body of evidence suggesting that psychedelic-like mystical experiences may be associated to therapeutic efficacy, not only in classic psychedelic-assisted therapy, but also in esketamine treatment.”

Ketamine as a potential cognitive enhancer in neurological disorders: evidence from preclinical and clinical studies (Rojas, et al, 2026)
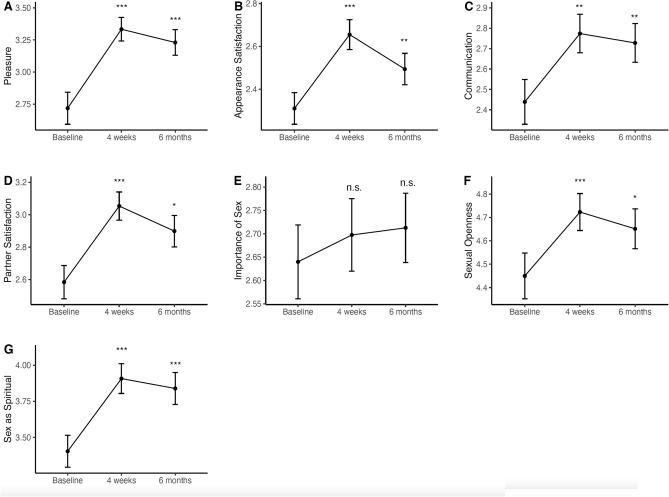
(2024)

(2026) Psychotherapy has proven efficacy across all severity levels, and it should be combined with antidepressants in severe episodes. In severe, psychotic and difficult to treat depressive episodes, strategies from the field of interventional psychiatry (ECT, rTMS, Esketamine) are effective. Complementary approaches such as physical activity/exercise, light therapy, or social therapy further enhance treatment outcomes.
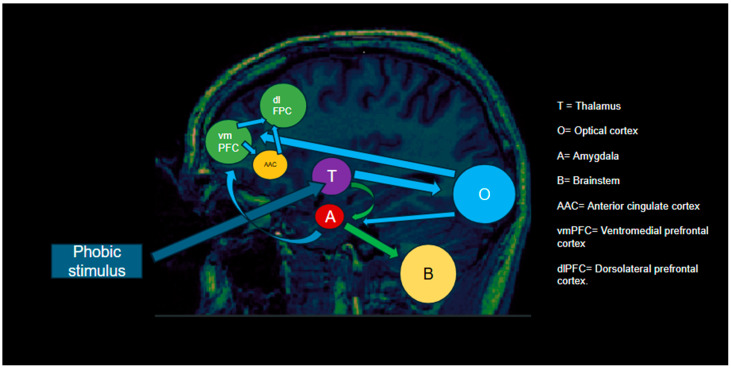
(2025) CBT consistently reduces subcortical activity and improves top-down regulation, restoring the balance between the cortical and subcortical systems... One potential alternative mechanism is neuroplasticity, as repeated cognitive and behavioral interventions in CBT may induce structural and functional changes over time, particularly in regions involved in self-referential processing and emotional regulation. Additionally, predictive coding models propose that anxiety is maintained by maladaptive anticipatory responses, and CBT may work by recalibrating these expectations, reducing excessive prediction errors in the brain’s fear-processing circuits. Finally, large-scale networks, such as the salience network, default mode network (DMN), and executive control network, play crucial roles in emotion regulation and cognitive control, and their interactions may be key in explaining the variability in neural responses observed across different anxiety disorder
(2026) The findings indicate that treating sleep problems might be a practical way to help improve mood and emotional regulation for those recovering from alcohol addiction.

(2026): "...esketamine appears to be cognitively safe in adults with treatment-resistant depression and may confer selective improvements, particularly in attention and processing speed, with more variable benefits in memory and executive functioning over sustained treatment. These effects may support functional recovery and complement esketamine's antidepressant action."

(2026):"Cognitive effects of intravenous Ketamine in treatment-resistant depression: A systematic review (Chavigny, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/42100880/ Subanesthetic IV ketamine appears to preserve and enhance specific cognitive functions in TRD, notably across processing speed, working memory, and executive control. These procognitive effects, particularly in executive control, may mediate ketamine's antisuicidal action."

(2026): "This comprehensive umbrella review demonstrates the importance of physical activity to reduce symptoms of depression and to have a positive impact on autonomic function. Further studies suggest that physical activity can also improve HRV in individuals with MDD."
How Slow Waves During Sleep Take Over to Clear Metabolic Trash (2026)
“Remission from major depression via treatment with CBT or medication is associated with changes in rsFC (resting state functional connectivity) that are mostly specific to the treatment modality, providing biological support for the clinical practice of switching between or combining these treatment approaches. Medication is associated with broadly inhibitory effects. In CBT remitters, the increase in rsFC strength between networks involved in cognitive control and attention provides biological support for the theorized mechanism of CBT. Reducing affective network connectivity with motor systems is a shared process important for remission with both CBT and medication.”(Dunlop, et al, 2017)
In this study of previously untreated adults with major depression, outcomes after 12 weeks of treatment with randomly assigned medication or CBT were associated with the degree of resting-state functional connectivity between brain regions involved in mood regulation—specifically, the SCC and 1) the left frontal operculum (incorporating the BA47 in the ventrolateral prefrontal cortex [VLPFC] and anterior insula); 2) the left ventromedial prefrontal cortex (BA 10); and 3) the dorsal midbrain. (2017)
Modulatory effects of ketamine on EEG source-based resting state connectivity in treatment resistant depression (Lees, et al, 2026)
Researchers write “A sample of 11,441 patients was analyzed, At-home, telehealth-supported ketamine administration was largely safe, well-tolerated, and associated with improvement in patients with depression. Strategies for combining psychedelic-oriented therapies with rigorous telehealth models, as explored here, may uniquely address barriers to mental health treatment.”
Brain Scans May Offer Clues About Depression Remission (Zagorski, 2023)
The researchers observed a stark difference in the scans of the participants after they received 12 weeks of treatment. In general, people who achieved remission following use of antidepressants showed reduced connectivity (electrical activity) between certain brain regions compared with baseline. In contrast, people who achieved remission following CBT had increased connectivity between these same regions. Notably, remission following CBT was associated with stronger connections between the brain regions that control executive function—the cognitive ability to process and prioritize information to complete a task—and attention. Executive function is often impaired in patients who are depressed, which can result in negative attitudes and beliefs being prioritized by the brain before positive ones, Dunlop explained. Cognitive training helps people to identify maladaptive thoughts and push these thoughts away.
Decoding the molecular network communication mechanism of ketamine’s antidepressant effects (Li, et al, 2026)
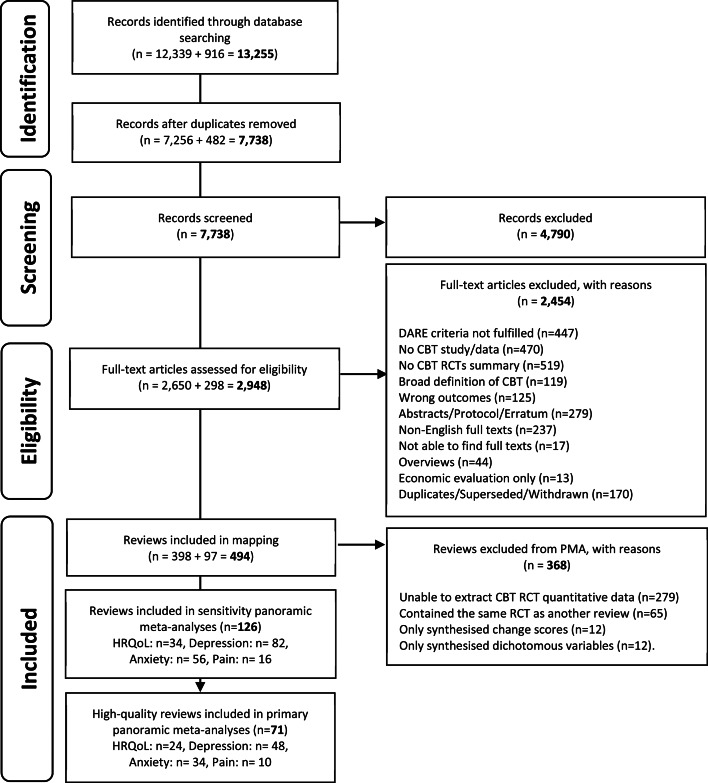
(2021): "Cognitive behavioural therapy (CBT) has more evidence supporting it than any other psychological therapy (David, Cristea, & Hofmann, 2018)."
Cognitive–behavioral therapy for management of mental health and stress-related disorders: Recent advances in techniques and technologies (2021): "The results of several randomized controlled trials indicated that CBT was effective for a variety of mental problems (e.g., anxiety disorder, attention deficit hypersensitivity disorder, bulimia nervosa, depression, hypochondriasis), physical conditions (e.g., chronic fatigue syndrome, fibromyalgia, irritable bowel syndrome, breast cancer), and behavioral problems (e.g., antisocial behaviors, drug abuse, gambling, overweight, smoking), at least in the short term"
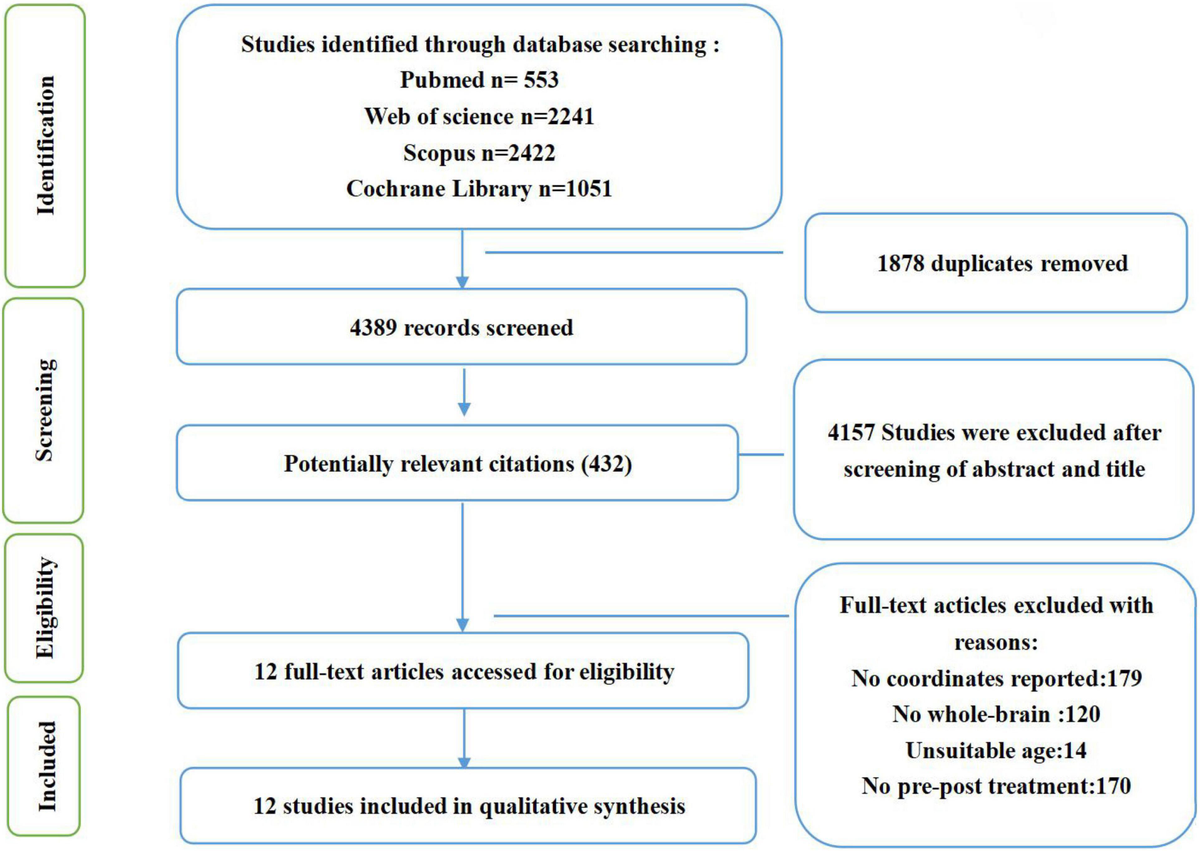
(2022):"The results revealed that the altered activation in the prefrontal cortex and precuneus were key regions related to the effects of CBT. Therefore, CBT may modulate the neural circuitry of emotion regulation. This finding provides recommendations for the rapidly developing literature."
Spotlight: "A Blueprint for Implementing Ketamine-Assisted Psychotherapy in Palliative Care: Design, Process, and Treatment Patterns of a Real-World Clinical Program" (Horowitz, et al, 2026) “...decades of preliminary research suggest that psychedelic-assisted psychotherapy (PAP), including ketamine-assisted psychotherapy (KAP), may alleviate the anxiety, depression, and existential distress…”
Teletherapy-based CBT has shown comparable, and in some cases superior, efficacy to traditional in-person therapy for depression [157,192,196]. Research has consistently demonstrated significant reductions in depressive symptoms and improved quality of life across diverse patient populations [128,148,173,190]. The flexibility and accessibility of teletherapy, further enhanced by digital tools, are key to its effectiveness, allowing tailored interventions, improved engagement, and better adherence [186]. To optimize teletherapy for personalized care, it is essential to incorporate individualized treatment planning [165], real-time digital monitoring and feedback [128], flexible and supportive communication options [163,188], and advanced technologies [179,181]. The inclusion of human support alongside digital interventions, as in [116,204], has been shown to improve outcomes, and personalized feedback, as emphasized by multiple researchers [171], ensures that treatment remains responsive to the evolving needs of patients.
Benefits of Cognitive Behavior Therapy with Neuroscience-informed Psychoeducation in Young Adult Patients: A Preliminary Study (2024)"Neuroscience-based psychoeducation has the potential of changing perception and enhancing the credibility of CBT and can bring better acceptance and outcome for the CBT process."
Ketamine-Induced Glutamatergic Mechanisms of Sleep and Wakefulness: Insights for Developing Novel Treatments for Disturbed Sleep and Mood (Duncan, et al, 2017) https://pmc.ncbi.nlm.nih.gov/articles/PMC5866161/ "Consistent with its effects on clock-associated molecules, ketamine alters the timing and amplitude of circadian activity patterns in rapid responders versus non-responders with MDD, suggesting that it affects mood-dependent central neural circuits.”
Ketamine Improves Anhedonic Phenotypes Across Species: Translational Evidence From the Probabilistic Reward Task (Bogdanov, et al, 2026) Ketamine is a promising treatment for people with depression who do not respond to standard therapies. In this study Ketamine restored reward responsiveness to normal levels within 24 hours, especially in people with elevated baseline anhedonia, suggesting a shared mechanism for reducing motivational deficits.
Ketamine as a Bridge Therapy: Reducing Acute in Hospital Settings (Lie, et al, 2026) “Ketamine's mechanism-of-action through mTORC1 is much faster than SSRI's downstream transcriptional regulation, leading to quicker relief of suicidal symptoms and the removal of the danger zone lag period. The current literature suggests that a controlled, supervised subanesthetic dose of Ketamine in a clinical setting has low risks of addiction or abuse…”
The Awake “Sleep” Loop: Why Attention Lapses Occur in ADHD (2026)
Baseline Pain Variability is Linked to Neural Reappraisal and Catastrophizing Improvement Following Cognitive Behavioral Therapy in Fibromyalgia (2026) "Pain catastrophizing up-regulates chronic pain and is a central target of cognitive behavioral therapy (CBT)."
Brain scans reveal how poor sleep fuels negative emotions in alcohol addiction (2026)
The effect of glutamatergic modulators on sleep behavior and architecture in depressive disorders: A systematic review (Valentino, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/41763189/ Our findings indicate that glutamatergic modulators, primarily ketamine, are associated with improvement across several sleep behaviors commensurate in MDD, suggesting that mechanisms subserving sleep are potential targets for depression treatment.
Psilocybin or Nicotine Patch for Smoking Cessation A Pilot Randomized Clinical Trial (Johnson, et al, 2026) https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2846155?resultClick=1 In this pilot randomized clinical trial, 1 dose of psilocybin with manualized CBT significantly increased long-term abstinence compared with nicotine patch treatment with CBT. Psilocybin abstinence rates were higher than typical treatments, suggesting promise for tobacco smoking cessation
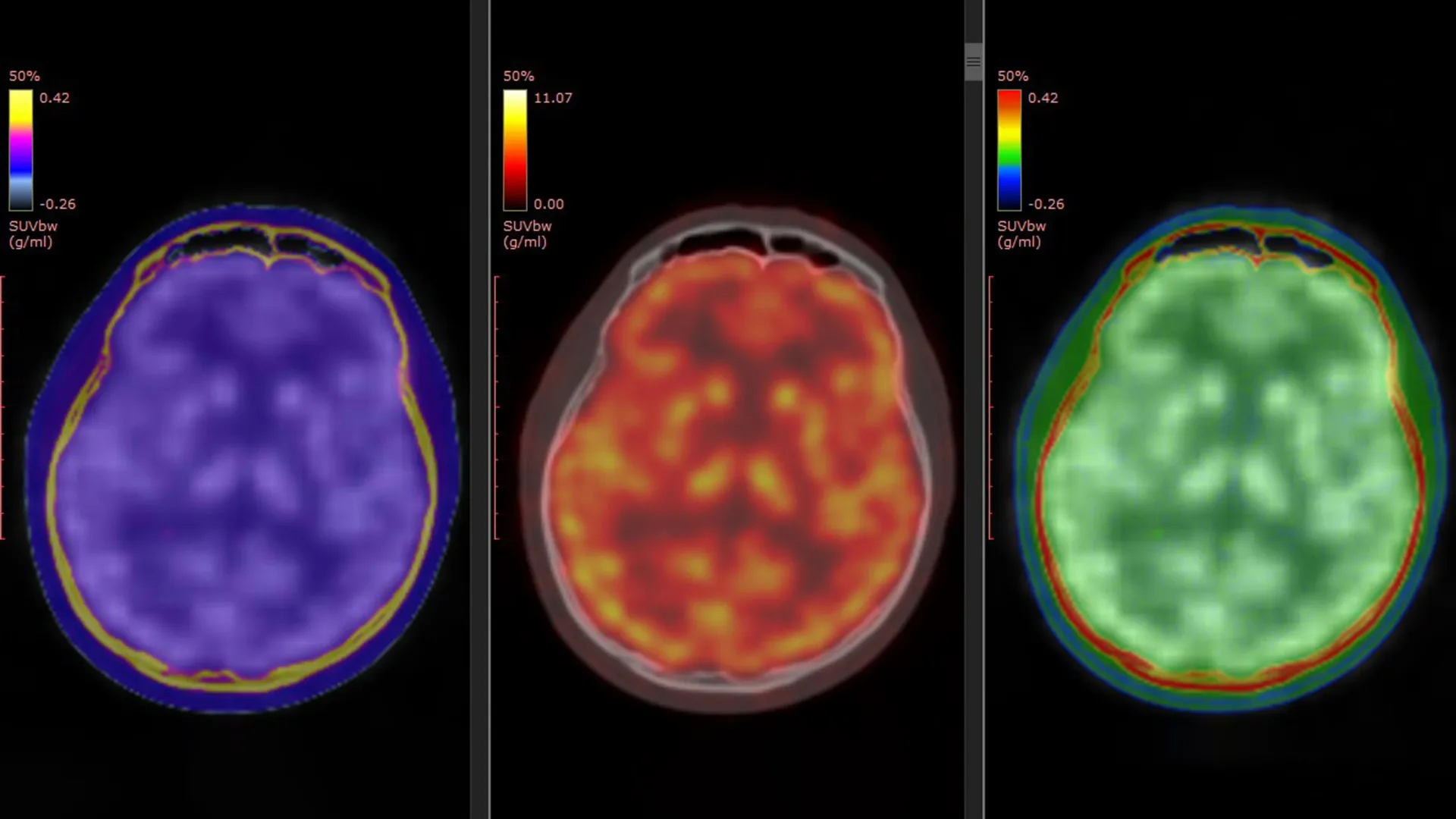
(2026) "ketamine reshapes its activity in specific brain regions tied to mood and reward. These shifts strongly matched improvements in patients’ symptoms."
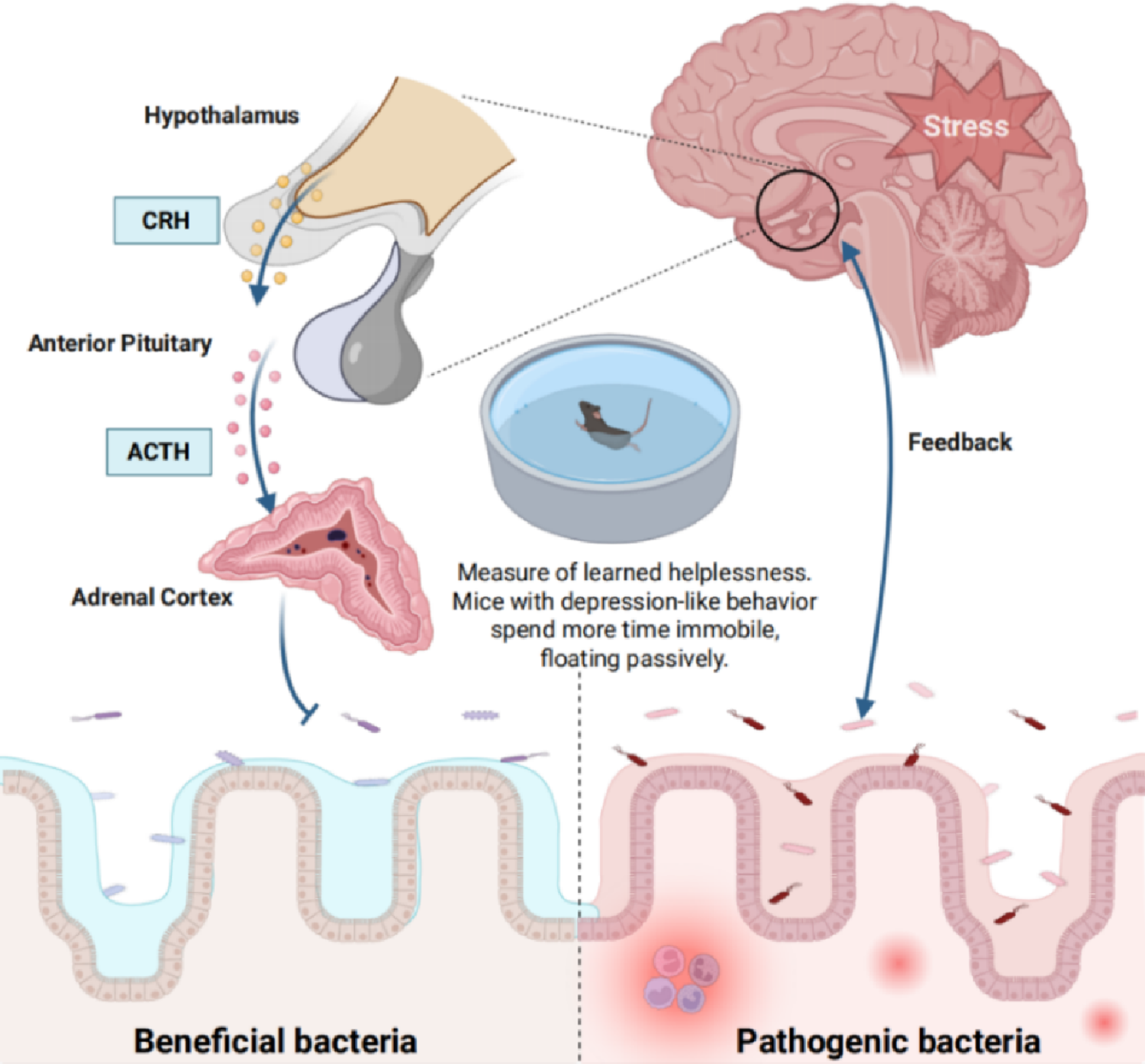
(2025) There is a complex, bidirectional interaction between the gut microbiota and the central nervous system, known as the gut-brain axis. Esketamine, as the right-handed isomer of ketamine, has been approved by the US FDA for the treatment of treatment-resistant depression (TRD), and its rapid antidepressant effect may involve modulation of gut microbiota. In addition, other ketamine isomers (such as R-ketamine) and racemic mixtures (R, S-ketamine) may also affect the gut microbiota through different pathways. This article reviews the potential regulatory mechanisms of ketamine and its isomers on gut microbiota, including anti-inflammatory effects, regulation of neurotransmitter metabolism, and intestinal barrier repair.
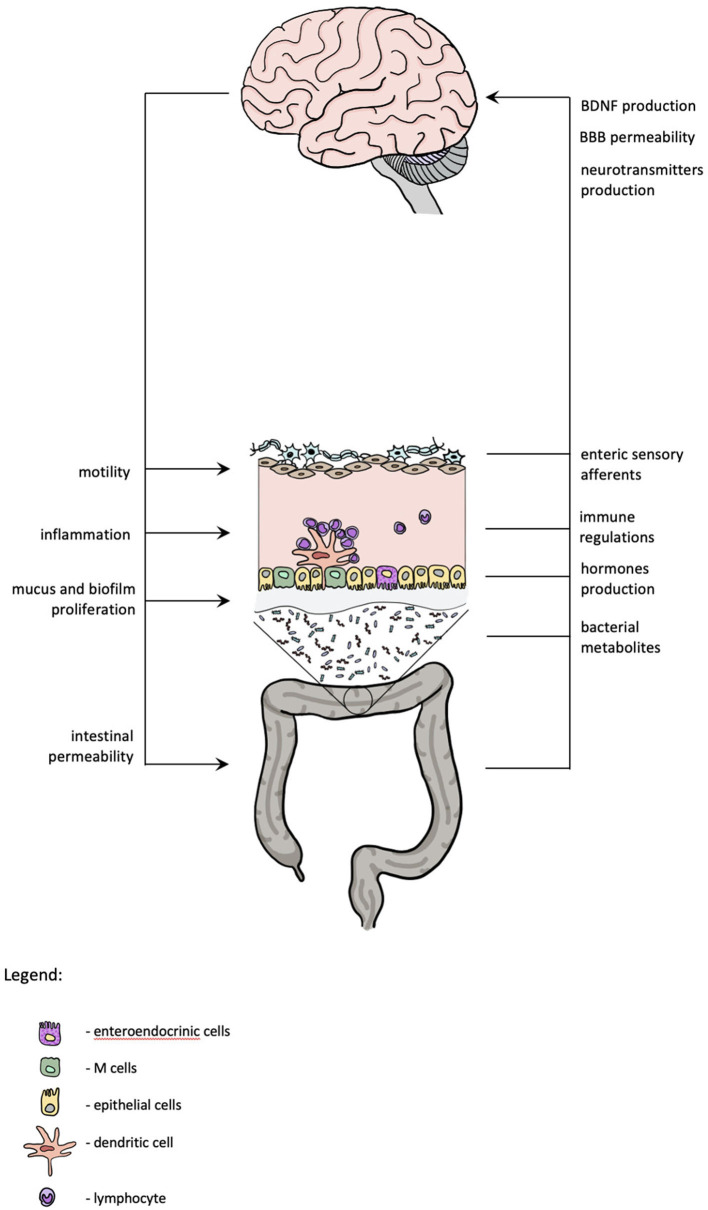
(2021): Preliminary study suggests "Ketamine seems to restore bacteria producing the anti-inflammatory substance, butyrate, and reduce the number of bacteria associated with inflammatory processes in the gut. It increases the abundance of bacteria, previously reported as reduced in depression, and reduces the amount of bacteria, previously reported as increased in MDD. It also increases the abundance of probiotic bacteria known to produce an antidepressant effect."
The Brain-Gut Connection "Psychological interventions like CBT may also help to 'improve communications' between the big brain and the brain in our gut."
(2023) "Ketamine increases synaptic glutamate release by blocking NMDARs either on GABAergic or glutamatergic synapses. Blocking NMDARs on GABAergic neurons reduces their inhibitory input on glutamatergic neurons, and blocking NMDARs on glutamatergic neurons promotes their excitatory synaptic drive.The burst release of glutamate activates AMPARs on dopaminergic neurons, which leads to the activation of VDCC, causing two effects. First, increased dopamine release promotes D2R/D3R signalling, which can also be activated by ketamine. Secondly, enhanced BDNF/TrkB signalling results in increased extracellular free BDNF.Blockage of NMDARs on dopaminergic neurons by ketamine leads to the inactivation of eEF2 kinase. Such inactivation prevents the phosphorylation of eEF2, thereby reducing its content. The reduction of eEF2 prevents its inhibition of BDNF/TrkB signalling.Increased D2R/D3R signalling and BDNF/TrkB signalling activate downstream MEK/ERK and AKT/mTOR pathways, which drive the molecular machinery required for neuroplasticity and synaptogenesis.Inhibition of the noradrenaline transporter by ketamine prevents its uptake of noradrenaline at the gap junctions, leading to an increase in free noradrenaline. Both extracellular serotonin and acetylcholine are increased caused by the action of ketamine on their receptors.All these neurotransmitters and BDNF are essential in the ketamine pathway and can be produced or promoted by gut microbes. In turn, some can stimulate or inhibit the growth of certain gut bacteria."

(2026):"Affective disorders such as depression, anxiety disorders and suicidality are major contributors to global psychiatry. The "chemical imbalance" theory has been traditionally used; however recent research suggests that neurotransmitter dysfunction may represent an important early contributor within a broader, bidirectional cascade of cellular changes. Stress responses and neural circuits are disrupted by dysregulation of the serotonergic, noradrenergic, dopaminergic, GABAergic, and glutamatergic systems, which leads to oxidative stress, excitotoxicity, neuroinflammation, and decreased trophic support. Reduced brain-derived neurotrophic factor (BDNF) signaling, dendritic retraction, synapse loss, and apoptotic susceptibility are the common pathways that result in both amygdala hyperactivity and structural atrophy in the hippocampus and prefrontal cortex. Rumination, fear, anhedonia, cognitive impairment, and suicidal ideation are clinical manifestations of the ensuing circuit failure. This study proposes a unified model of pathogenesis in which increasing cellular damage is driven by neurotransmitter dysregulation, integrating evidence from both the neurochemical and cellular domains. Reassessing the delayed but plasticity-enhancing benefits of SSRIs and SNRIs, the quick synaptic repair brought about by NMDA antagonists like ketamine, and the potential of new drugs that target oxidative stress, inflammation, and glutamate receptor subtypes are some of the therapeutic implications. Lastly, it is highlighted that developing biomarkers for oxidative damage and neuroinflammation is an essential next step in the development of precision psychiatry. This paradigm aims to shift the emphasis from regulating neurotransmitters to promoting cellular resilience and rebuilding brain circuits in order to reimagine the future of treatment for depression, anxiety, and suicidality."
Effect of Ketamine on Reward Processing in Depressive Disorders: A Systematic Review of Neuroimaging Studies (Faisal, et al, 2026) "This systematic review found that ketamine administration is associated with neurofunctional changes in reward-related circuitry in adults with MDD/TRD, most consistently involving the ventral striatum/NAc and connected ACC–prefrontal networks. “

Inflammation and treatment strategies for suicidal behavior (2026) Individuals w/ suicidal behaviour exhibit elevated pro-inflammatory cytokines (interleukin-6, interleukin-1β, tumour necrosis factor-α), C-reactive protein (CRP), and chemokines in blood, CSF, and brain tissue. Several immunomodulatory treatments - including lithium, ketamine/esketamine show promise in reducing inflammation-linked to suicidal risk. #ketamine #esketamine #suicide #mentalhealth #psychedelics https://pubmed.ncbi.nlm.nih.gov/42059933/

Intranasal Ketamine for Existential Distress in Advanced Cancer (2026) https://pubmed.ncbi.nlm.nih.gov/42055096/ Intranasal ketamine was associated with clinically meaningful improvements in existential distress in individuals with advanced cancer being treated for depression. Ketamine may have relevance as a single agent for multidimensional distress in palliative care.
Measuring the psychoactive effects of ketamine in alcohol use disorder: When assessment shapes experience (McAnaulty & Garrl, 2026) https://

Experiences of Awe Mediate Ketamine’s Antidepressant Effects: Findings From a Randomized Controlled Trial in Treatment-Resistant Depression (Aepfelbacher, et al, 2024) infusion strongly induced heightened feelings of awe, and these experiences consistently mediated depression outcomes over a 1- to 30-day period, unlike general dissociative side effects. The specific awe-inspiring properties of ketamine may contribute to its antidepressant effects.
Awe as a Pathway to Mental and Physical Health (2022)

Mystical Experience Induced by Esketamine Treatment: A Real-World Observational Study (Mallevays, et al., 2026) https://pubmed.ncbi.nlm.nih.gov/41959772/ “These findings add to the growing body of evidence suggesting that psychedelic-like mystical experiences may be associated to therapeutic efficacy, not only in classic psychedelic-assisted therapy, but also in esketamine treatment.”

(2023): "All participants' symptoms declined throughout treatment. Psychedelic treatment participants saw a larger, more consistent decrease. Researchers conclude that KAPT may be effective for treating chronic pain/MDD comorbidity, anxiety and Post-Traumatic Stress Disorder (PTSD). Findings imply that the psychedelic approach may be more effective."

Evidence in practice: implementing KAT in indigenous health services (Lovely, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/42100772/ #ketamine #ketaminetherapy Findings demonstrated notable improvements in symptoms of #depression #anxiety and #ptsd with participants reporting increased emotional regulation and stronger cultural connections.

(2023): "We found that the ketamine administration caused an altered state of consciousness and changes in systemic physiology (e.g. increase in pulse rate and electrodermal activity). Furthermore, ketamine led to a brain-wide reduction in the fractional amplitude of low frequency fluctuations, and a decrease in the global brain connectivity of the prefrontal region. Lastly, we provide preliminary evidence that a combination of neural and physiological metrics may serve as predictors of subjective mystical experiences and reductions in depressive symptomatology. Overall, our study demonstrated the successful application of fNIRS neuroimaging to study the physiological effects of the psychoactive substance ketamine in humans, and can be regarded as an important step toward larger scale clinical fNIRS studies that can quantify the impact of psychedelics on the brain in standard clinical settings."

(2023): "Patients reported several esketamine effects with psychotherapeutic potential, such as increased openness, detachment, an interruption of negativity, and mystical-type experiences. These experiences deserve to be explored further to enhance treatment outcomes in patients with TRD. Given the frequency and severity of the perceived distress, we identify a need for additional support in all stages of esketamine treatment."

(2022): "The mystical experience is a potential psychological mechanism to influence outcome in psychedelic therapy. It includes features such as oceanic boundlessness, ego dissolution, and universal interconnectedness, which have been closely linked to both symptom reduction and improved quality of life. In this review, 12 studies of psychedelic therapy utilizing psilocybin, ayahuasca, or ketamine were analyzed for association between mystical experience and symptom reduction, in areas as diverse as cancer-related distress, substance use disorder, and depressive disorders to include treatment-resistant. Ten of the twelve established a significant association of correlation, mediation, and/or prediction."

Cognitive Behavioral Therapy Following Esketamine for Major Depression and Suicidal Ideation for Relapse Prevention: The CBT-ENDURE Randomized Trial (Wilkinson, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/42095692/ This study demonstrates the feasibility and the effectiveness of combining CBT with esketamine to reduce SI and prevent relapse in patients with MDSI.
Ketamine combined with psychotherapy for treatment-resistant depression: Real-world outcomes and the role of subjective experience (Cohen, et al, 2026)
Ketamine-Occasioned Mystical Experience in Veterans with Treatment-Resistant Depression: A Retrospective Exploratory Analysis (2025) "These findings suggest that ketamine can occasion mystical experiences in veterans with treatment-resistant depression. Future studies should further explore the mystical-type effects of ketamine as a potential contributor to its therapeutic effect in treatment-resistant depression."

An ongoing review of the literature

(2026):"findings indicate that cognitive-behavioral strategies have been incorporated into psychedelic-assisted interventions in diverse ways, across different phases of treatment and with distinct therapeutic purposes."

Ketamine as a potential cognitive enhancer in neurological disorders: evidence from preclinical and clinical studies (Rojas, et al, 2026)

(2024)
Psychedelics May Enhance Intimacy, Attraction, and Sexual Expression (2025)


https://www.jsatjournal.com/article/S0740-5472(02)00275-1/fulltext
"Ketamine psychotherapy for heroin addiction: immediate effects and two-year follow-up" (2002)
Advancing cancer neuroscience through stress modulation: Interdisciplinary potential of psilocybin and ketamine (Courtes, et al, 2026)
Progress, potential and pitfalls of ketamine as a treatment for Depression and related disorders (Orsini, et al, 2026)
Psychedelic-Assisted Psychotherapy and Mindfulness-Based Cognitive Therapy: Potential Synergies (2023) - clear role in supporting psychedelic process, particularly in psychedelic-assisted psychotherapy, likely to prove extremely useful in the preparation, dosing and integration phases.
Ketamine combined with psychotherapy for treatment-resistant depression: Real-world outcomes and the role of subjective experience (Cohen, et al, 2026)

The findings of this systematic review and meta-analysis suggest that single and repeated intravenous ketamine infusions are efficacious in reducing suicidal and depressive symptoms in patients with an MDE in the acute phase “Ketamine Infusions and Rapid Reduction of Suicidal and Depressive Symptoms in Major Depressive Episode: A Systematic Review and Meta-Analysis” (Shim, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/420901
Inflammatory models of depression in rodents and humans (Markov, et al, 2025)
A naturalistic inventory of prescribing practices, safety, and adverse effects (Stuart, et al, 2025) Non-IV forms of ketamine were commonly used, and the survey reported a favorable safety profile for ketamine. Non-IV Ketamine was reported to be safely utilized in a clinic setting with minimal monitoring and safety equipment, or at times, for home use. strict universal regulations for all formulations may unnecessarily limit patient access.
Oxidative Stress in Treatment-Resistant and Refractory Depression: A Hidden Therapeutic Target? (Winczewska et al., 2026)

(2025): "A better response to ketamine was not predictive of a better response to esketamine in our case series. A deeper insight into the side effects of the treatments (eg, dissociation) and into the clinical history of the patients would be helpful in better understanding the relationship between the 2 treatments."(Carminati, et al, 2025)
From Monoamine Deficits to Multiscale Plasticity: Twenty-Five Years of Ketamine and the Neurophysiology of Depression (Bulek, et al, 2026)
“improvement in depressive symptoms was observed, despite their severity, in a sample submitted to multiple previous pharmacological strategies.This retrospective study evaluated ketamine infusions combined with psychotherapy in nine patients with treatment-resistant depression at a general hospital. After eight weeks, all participants improved, scores shifting from severe to moderate. Overall, 44% responded to treatment”

(2026): "Subcutaneous, flexible-dosed, racemic ketamine over four weeks showed beneficial effects on suicidal ideation scores. "

esketamine was used adjunctively with ongoing oral antidepressants. Intranasal esketamine in treatment-resistant #depression long-term dosing patterns and clinical outcomes in a 5-year observational study (Cuomo, et al, 2026) https://pubmed.ncbi.nlm.nih.gov/42052285/ associated with sustained symptom improvement and a favorable long-term safety profile among patients who continued treatment, with dosing evolving from induction to individualized maintenance schedules up to 260 weeks
Meditation and psychedelics (including ketamine) facilitate similar types of mystical, psychological, and philosophical-existential insights predictive of wellbeing: a qualitative-quantitative approach (Jylkkä, et al, 2025)
Unfolding States of Mind: A Dissociative- Psychedelic Model of ketamine psychotherapy in palliativecare (Gonçalves Campolina & Tuena de Oliveira, 2025) "a compassionate, pragmatic, theoretically grounded approach to relieving psychological & existential suffering in palliative care integrating neurobiological insights w/ psychotherapeutic processes- a flexible, patient-centered framework for enhancing meaning, emotional resolution, quality of life at the end of life.
A long, strange trip: Ketamine treatment in psychiatry (Nutt, et al, 2025) "...mystical experiences were strongly related to immediate and sustained psychiatric benefits at the group level and on an individual, session-by-session basis across the six doses, providing mechanistic support for ketamine-psychotherapy pairings."
Efficacy and safety of ketamine maintenance therapy in treatment-resistant depression: A systematic review of treatment protocols and clinical outcomes (Al-Garni, et al, 2025) "Concurrent psychotherapy improved treatment maintenance. Adverse events were generally mild to moderate... Ketamine maintenance therapy shows promise as a treatment option for TRD, with regular dosing schedules and early intervention associated with optimal outcomes."

Ketamine-related neural changes in treatment-resistant depression: A multimodal synthesis of fMRI and PET studies (2026) findings suggest that ketamine-related effects were frequently reported in subcortical regions, alongside more distributed and context-dependent effects across cortical systems, including prefrontal and anterior cingulate regions. Network-level summaries further suggested involvement of default-mode, ventral attention, and visual systems. https://pubmed.ncbi.nlm.nih.gov/420615

pubmed.ncbi.nlm.nih.gov/42066082/ #ketamine TrkB/mGluR5 cross-talk underlies a synaptic metaplasticity mechanism of ketamine (2026)
2026 Psychedelics Documentary
The heart of the self: An interoceptive perspective on the psychotherapeutic process (2026) "Psychotherapy can be refined through neurocognitive models of embodied self-processing."


(2026) Depression is driven by dysfunction in discrete neural circuits, but a deeper understanding of the underlying molecular and synaptic mechanisms is needed to guide the development of therapeutics. Here, we decipher the mechanisms of action of the fast-acting antidepressant ketamine to enable the identification of G protein-coupled receptor (GPCR) antidepressant targets. We find that the behavioral effects of ketamine rely on mu-opioid receptors (MORs), which are enriched in somatostatin-expressing interneurons (Sst+ INs) in the medial prefrontal cortex (mPFC). Chronic stress drives presynaptic hypertrophy of mPFC Sst+ INs and excessive inhibition of pyramidal neurons, which is rescued by ketamine.

(2026) Baseline IL-6 may predict response to esketamine in TRD, highlighting the potential role of inflammation in treatment resistance and supporting biomarker-guided personalized interventions.
Repeated intranasal esketamine augmentation in treatment-resistant obsessive-compulsive disorder with comorbid major depressive disorder: a prospective case series (2026) “Repeated intranasal esketamine may offer a therapeutic window for patients with severe TR-OCD and comorbid MDD. These preliminary findings support further controlled studies to clarify its role, optimal administration, and integration with psychotherapy.”

New Antidepressant Development in the Treatment of Depression (Spiti, et al, 2026) "A breakthrough came with N-methyl-D-aspartate (NMDA) receptor antagonists such as ketamine and esketamine, which achieved fast-acting effects and shifted the focus to glutamatergic modulation. Other developments in this area include modulators such as partial agonists, positive allosteric modulators (PAMs), and negative allosteric modulators (NAMs). In addition, gamma-aminobutyric acid (GABA) modulation has gained attention, with neurosteroids such as zurolone (approved for postpartum depression [PPD]) representing a new therapeutic approach. Other new strategies target the opioid system, particularly kappa-opioid receptor (KOR) antagonism, whose role in the treatment of anhedonia and depression is being investigated. Psychedelics, including psilocybin, have come back into focus as potential treatments due to their ability to elicit rapid and sustained antidepressant effects via agonism of the serotonin 2A receptor (5-HT2A)"
From chronic pain to depression: Neurogenesis-driven microglial remodeling in the hippocampal dentate gyrus (2026) "findings reveal microglia-mediated hippocampal remodeling as a key mechanism linking chronic pain to mood disorders."

(2026): "Depression and chronic pain frequently co-occur, amplifying disease burden and complicating treatment. Shared mechanisms span immune, neurotransmitter, and neuroplastic domains. Neuroinflammation, characterized by elevated cytokines such as IL-6 (interleukin-6) and TNF-α (tumor necrosis factor-alpha), drives both mood dysregulation and nociplastic pain through microglial activation and central sensitization. Dysregulation of glutamate and gamma-aminobutyric acid (GABA) signaling contributes to excitatory-inhibitory imbalance, while altered BDNF (brain-derived neurotrophic factor) expression links neuroplasticity with pain amplification. Substance P and monoamine disturbances further integrate affective and somatic symptoms. Neuroimaging reveals overlapping dysfunction in prefrontal, cingulate, and limbic networks, providing a unifying framework for pain-emotion interactions. Psychological and social factors, including maladaptive cognitions, emotion regulation deficits, and reduced social support, exacerbate this bidirectional relationship. Clinically, tricyclic antidepressants and SNRIs (serotonin-norepinephrine reuptake inhibitors) demonstrate superior analgesic efficacy compared with SSRIs, particularly in neuropathic pain, fibromyalgia, and irritable bowel syndrome. Novel agents such as ketamine and esketamine show rapid antidepressant and potential analgesic effects. Neuromodulation strategies (rTMS (repetitive transcranial magnetic stimulation), tDCS (transcranial direct current stimulation)) and psychological interventions (CBT (cognitive behavioral therapy), mindfulness, ACT (acceptance and commitment therapy)) further enhance outcomes. Together, these findings support a precision medicine approach that integrates biological, psychological, and social determinants. Targeting convergent mechanisms may reduce symptom burden, improve treatment responsiveness, and ultimately enhance quality of life in patients with comorbid depression and chronic pain."

Ketamine Psychedelic Harm Reduction

Table of Contents
From the journal Innovation in April 2026: Quantum evidence of nonlocal consciousness during clinical death (2026) "If consciousness can operate under quantum principles, then the boundaries between life, death, and cognition are far more permeable than current science allows... NDEs positively correlated with neuroplasticity during Cardiac Arrest. Biomarker models explained up to 56.8% of the variance in recall. These findings compel a radical rethinking of clinical death: consciousness may persist—quantum-bound, detectable, and not yet defeated.
Certain anesthetics and psychoactive agents, especially ketamine—a
dissociative NMDA antagonist—are well-documented to induce phenomenological states that closely mimic spontaneous NDEs. These include out-of-body experiences, time distortion, depersonalization, and profound tranquility or transcendence.104–106 A large-scale semantic analysis of subjective reports has confirmed that ketamine-induced states are more similar to NDEs than those associated with serotonergic psychedelics.105 These similarities support the hypothesis that shared neurochemical mechanisms—such as transient NMDA receptor blockade and glutamatergic dysregulation under extreme stress—may underpin NDEs. One speculation is that the dying brain might endogenously release ketamine-like compounds or enter a disinhibited cortical state, temporarily supporting heightened internal awareness. These findings reintroduce anesthesiology into broader debates on the neural correlates of consciousness, including theories that embrace non-classical processes such as quantum brain dynamics. Notably, our study found correlations between verified quantum entanglement effects and conscious recall, lending empirical support to theoretical models—such as the Hameroff and Penrose (2014) theory57—that attempt to explain how awareness might emerge under otherwise suppressive conditions."

(2024): "Cognitive behavioral therapy, rooted in exposure therapy, is currently the primary approach employed in the treatment of anxiety-related conditions, including post-traumatic stress disorder (PTSD)… These findings contribute to our understanding of the underlying mechanisms of remote cued fear extinction, thereby offering a theoretical foundation and identifying potential targets for the intervention and treatment of PTSD.

(2022): "Our primary reasons for advocating for cognitive-behavioral approaches include, (1) they avoid issues of cultural insensitivity, (2) they make minimal speculative assumptions about the nature of the mind and reality, (3) they have the largest base of empirical support for their safety and effectiveness outside of psychedelic therapy. We then propose several concepts from cognitive-behavioral therapies such as CBT, DBT, and ACT that can usefully inform the preparation, session, and integration phases of psychedelic psychotherapy. Overall, while there are many sources from which psychedelic psychotherapy could draw, we argue that current gold-standard, evidence-based psychotherapeutic paradigms provide the best starting point in terms of safety and efficacy."
Learning to Let Go: A Cognitive-Behavioral Model of How Psychedelic Therapy Promotes Acceptance (Wolff, et al, 2020): "This article presents a conceptual model that specifies potential psychological mechanisms underlying such change, and that shows substantial parallels between psychedelic therapy and cognitive behavioral therapy: We propose that in the carefully controlled context of psychedelic therapy as applied in contemporary clinical research, psychedelic-induced belief relaxation can increase motivation for acceptance via operant conditioning, thus engendering episodes of relatively avoidance-free exposure to greatly intensified private events. Under these unique learning conditions, relaxed avoidance-related beliefs can be exposed to corrective information and become revised accordingly, which may explain long-term increases in acceptance and corresponding reductions in psychopathology."
Psychedelic-Assisted Psychotherapy—A Systematic Review of Associated Psychological Interventions (Cavarra, et al, 2022) "In a way, psychedelics seem to open a window of flexibility (Kuypers et al., 2016) that may relax higher level priors and increase sensitivity to bottom-up information (Carhart-Harris et al., 2018b; Carhart-Harris and Friston, 2019). In the context of psychotherapy, this could imply that patients are offered a window of opportunity to become more effective in modifying rigid behaviors, thought patterns, and emotional reactions and that psychotherapy itself must be carefully honed to take advantage of this fertile state."
Cognitive Behavioral Therapy, Ketamine, and Combination Treatment for Depression: Impressions of Credibility in Participants with Self-Reported Depressive Symptoms (Earleywine, et al, 2020)
"Over 500 participants with depressive symptoms read descriptions of CBT, ketamine, and a treatment that combined the two. Descriptions included pros and cons of each approach. Participants found the combination treatment more credible than ketamine but no better than CBT alone. They rated the credibility of CBT alone significantly higher than ketamine alone. Participants with psychotherapy experience tended to view ketamine as less credible than those who did not report previous psychotherapy. Depression scores did not covary with credibility ratings for any treatment. Despite media coverage and Internet claims, potential clients are cautious about ketamine. These results suggest that providing descriptions of treatments might help reveal important information about their credibility to potential clients."

(2021): "This proof-of-concept study provides preliminary data indicating that CBT may sustain the antidepressant effects of ketamine in TRD."
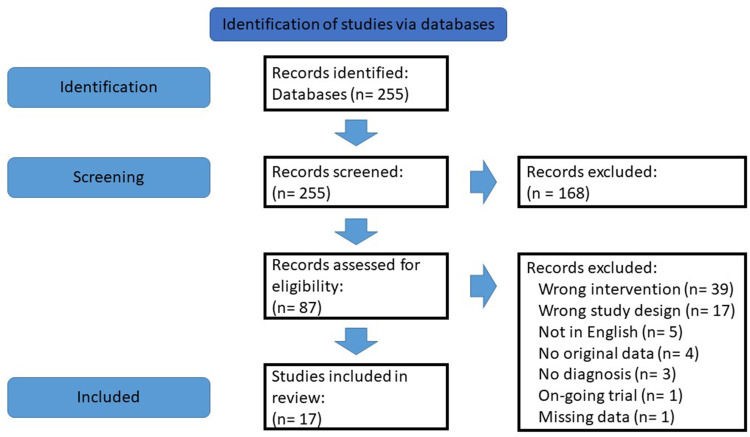
(2022): "The use of Ketamine Assisted Psychotherapy (KAP) can potentially fulfil the unmet clinical need for an effective treatment for multiple complex and often comorbid pain, psychological, and substance use disorders. Ketamine’s demonstrated ability to produce antidepressant and anxiolytic effects likely interacts with the processes involved in psychotherapy, ideally as a conduit for rapid-change, increasing treatment engagement and adherence, building the therapeutic alliance, and lowering defensiveness by providing reprieves from distressing symptomology while inducing transpersonal experiences at higher doses. Continued engagement in psychotherapy after ketamine administration may prolong the often-transient effects of ketamine and allow for the integration of psychological insights into everyday functioning. While at present there is no standard approach to the application of KAP, it is important to prepare and support the patient during ketamine administration and to offer follow-up psychotherapy sessions to maintain positive effects and delay or eliminate relapse. As KAP research continues to evolve, a focus on increasing the duration of positive effects may lead to effective interventions and maintenance programs, improving KAP such that it becomes an effective, long-lasting treatment for complex, resistant, and chronic conditions for people living with pain, mental health, and substance use disorders. // The theorized effectiveness of ketamine in psychotherapy is based on: (a) increased access to traumatic memory via enhanced synaptic connectivity; (b) decreased central sensitization via downregulation of the prefrontal cortex, and (c) enhanced extinction of previously paired pain-related memories.21 Therefore, KAP can utilize a dosage escalation strategy to achieve different levels of trance, increasing to full out-of-body experiences.23"

(2019): "Currently, ketamine is the only legal psychedelic medicine available to mental health providers for the treatment of emotional suffering. Over the past several years, ketamine has come into psychiatric use as an intervention for treatment resistant depression (TRD), administered intravenously without a psychotherapeutic component. In these settings, ketamine's psychedelic effects are viewed as undesirable "side effects." In contrast, we believe ketamine can benefit patients with a wide variety of diagnoses when administered with psychotherapy and using its psychedelic properties without need for intravenous (IV) access. Its proven safety over decades of use makes it ideal for office and supervised at-home use. The unique experience that ketamine facilitates with its biological, experiential, and psychological impacts has been tailored to optimize office-based treatment evolving into a method that we call Ketamine Assisted Psychotherapy (KAP). This article is the first to explore KAP within an analytical framework examining three distinct practices that use similar methods. Here, we present demographic and outcome data from 235 patients. Our findings suggest that KAP is an effective method for decreasing depression and anxiety in a private practice setting, especially for older patients and those with severe symptom burden."



Real Stories of Using Ketamine for Depression, Anxiety, PTSD (2025)
The anesthetic ketamine has skyrocketed in popularity as a fast, effective, often expensive treatment for ADHD comorbidities like depression, anxiety, PTSD, and more. Here, readers share their experiences.
The Therapeutic Effects of Ketamine in Mental Health Disorders: A Narrative Review (2022) "Ketamine, a non-competitive N-methyl-d-aspartate receptor antagonist, is commonly used as an anesthetic and analgesic but has recently shown promising research in treating certain psychiatric conditions such as depression, post-traumatic stress disorder (PTSD), suicidal ideation, and substance use disorder."
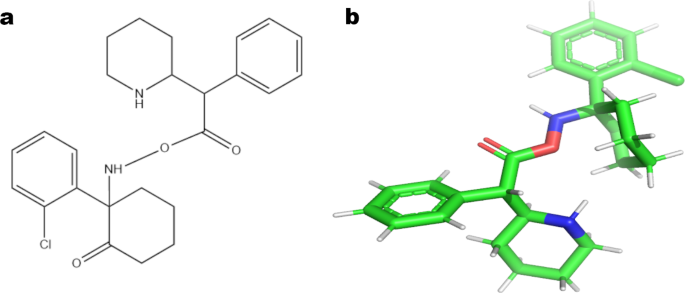
(2025): "Major depressive disorder (MDD) and Attention-deficit hyperactivity disorder (ADHD) are pervasive psychiatric disorders characterized by impaired memory, sustained attention/motivation, and depression. FDA-approved Ketamine is an antidepressant drug but it affects cognitive abilities. Methylphenidate is the drug used for the treatment of ADHD. Chronic treatment overcomes attention and mental problems but causes depression. In the current study, we have made ketamine-methylphenidate conjugate to treat/reduce side effects to treat both MDD and ADHD. // It is worth mentioning that serotonergic synapses and pathways of TPH2 are the classical signaling pathways not only in ADHD but also in MDD, therefore they are considered also the current hot directions for studying neurotransmitter dysregulation in attention and mood disorders.
“It is now widely accepted that ketamine is an effective and fast-acting antidepressant, proven to be beneficial for a variety of depressed patients” - Scheuing et al. (2015) National Institute of Mental Health.

A comprehensive review of the clinical progress of #esketamine From anesthesia to antidepressant therapy (Hu, et al, 2016) https://pubmed.ncbi.nlm.nih.gov/42065202/ Esketamine exerts its effects primarily through noncompetitive antagonism of N-methyl-D-aspartate receptors, leading to rapid modulation of glutamatergic signaling and neuroplasticity intravenous & intranasal esketamine have demonstrated rapid antidepressant effects in treatment-resistant depression, with response rates of 50% to 70% within 24 hours.
Michael Pollan follows up "How to Change Your Mind", now also a streaming series, with a new book on consciousness.

(2026): “findings suggest that mental habits play a significant role in shaping a person’s emotional experience…people create their own realities through the types of thoughts that they have. Individuals prone to negative affect seem to be contributing to their negative affect by choosing to think about problems and uncertainties under default conditions —findings could point to ways that pessimistic ways of living could be changed."




Personalized Multimodal and Opioid-Sparing Analgesia for Postoperative Pain Management: Enhancing Recovery and Addressing the Post-Discharge Gap (Sezerano, et al, 2026) includes ketamine and cognitive behavioral therapy for pain management https://pubmed.ncbi.nlm.nih.gov/420171



Repeated intranasal #esketamine augmentation in treatment-resistant obsessive-compulsive disorder with comorbid major depressive disorder: a prospective case series (2026) “Repeated intranasal esketamine may offer a therapeutic window for patients with severe TR-OCD and comorbid MDD. These preliminary findings support further controlled studies to clarify its role, optimal administration, and integration with psychotherapy.”

(2023): "Higher levels of media exposure reduced the mystical/emotional qualities of subsequent psychedelic ketamine experiences, overpowering standard intention-setting practices and altering therapeutic outcomes. Qualitative data from 24 additional patients yielded eight further spontaneous reports of past environmental exposures manifesting as visual hallucinations during ketamine experiences. We identified similar examples of imprinting with diverse psychoactive drugs in past publications, including in the first-ever report of ketamine in human subjects, as well as analogous processes known to underly dreaming."

(2024): "Esketamine enhanced psychological engagement with a daily MBI, compared to placebo, and led to transient decreases in alcohol cravings. Esketamine also resulted in significantly greater mystical experiences and dissociative states compared to placebo."

(2023): "We found that the ketamine administration caused an altered state of consciousness and changes in systemic physiology (e.g. increase in pulse rate and electrodermal activity). Furthermore, ketamine led to a brain-wide reduction in the fractional amplitude of low frequency fluctuations, and a decrease in the global brain connectivity of the prefrontal region. Lastly, we provide preliminary evidence that a combination of neural and physiological metrics may serve as predictors of subjective mystical experiences and reductions in depressive symptomatology. Overall, our study demonstrated the successful application of fNIRS neuroimaging to study the physiological effects of the psychoactive substance ketamine in humans, and can be regarded as an important step toward larger scale clinical fNIRS studies that can quantify the impact of psychedelics on the brain in standard clinical settings."

A deeper dive